What gets into the brain and what doesn’t is strictly regulated. Researchers at the Faculty of Medicine at the University of Freiburg have now studied phagocytes that coat the blood vessels in the brain and reinforce the blood-brain barrier. As the scientists from the Institute of Neuropathology at the Medical Center – University of Freiburg together with an international research team have shown, these cells only mature fully after birth according to a defined step-by-step developmental program. Until now, it had been assumed that this process was completed during embryonic development. Their studies, which were published in the journal Nature on April 20, 2022, were initially carried out on genetically modified mouse lines and were confirmed on human samples. They are expected to provide important insights into the development and treatment of diseases of the brain.


New discoveries about the origin of the brain’s immune system
Important immune cells in the brain’s blood vessels do not mature until after birth
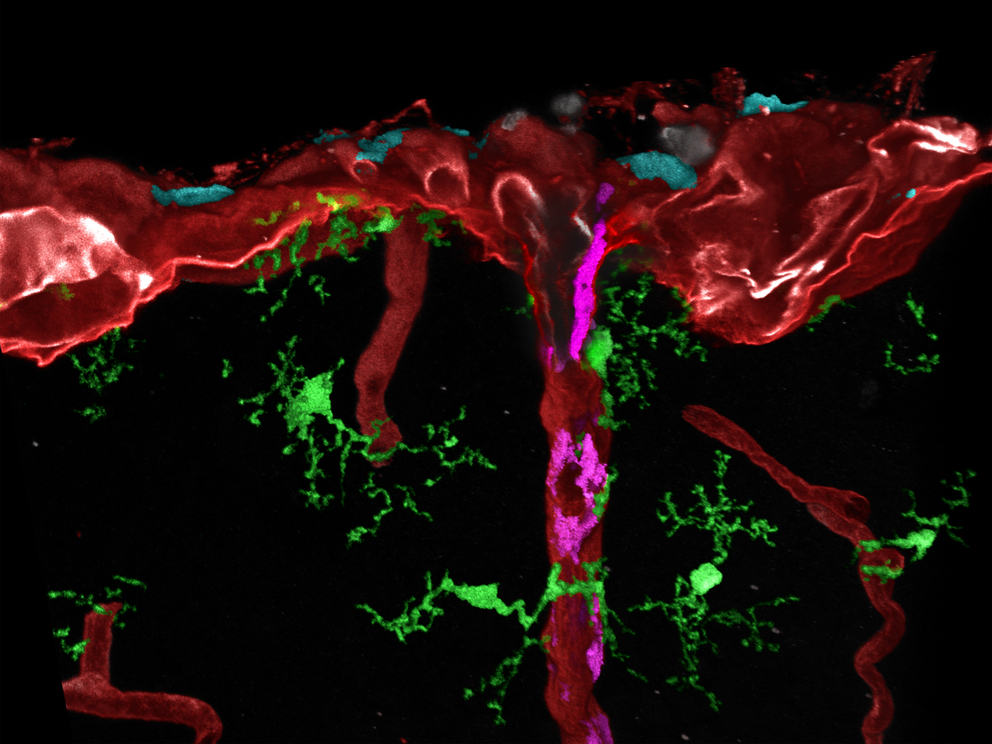
Post-processed microscopic image of different tissue macrophages (cyan, magenta or green) in mouse brain. Macrophages (magenta) at blood vessels are formed by migration of macrophages (cyan) from the meninges. Image: Medical Center – University of Freiburg / Dr. Lukas Amann
“We were able to show that the immune cells we studied migrate from the cerebral membrane to the blood vessels in the brain shortly before birth and mature there. This process is probably not completed until weeks after birth and could partly explain why the brain is so vulnerable at the beginning of life,” says Prof. Dr. Marco Prinz, Medical Director of the Institute of Neuropathology at the Medical Center – University of Freiburg and head of the Collaborative Research Center/Transregio 167 - NeuroMac and member of the Cluster of Excellence CIBSS -Centre for Integrative Biological Signalling Studies at the University of Freiburg. “The late timing of the maturation of the phagocytes, also called macrophages, was very surprising to us, since the precursor cells are already present in the brain long before,” says Prinz. In addition, the scientists were able to show for the first time that the vessels, as structure-giving cells of the brain, send important signals for normal development of the brain’s macrophages.
The blood-brain barrier is formed by cells on the blood vessels of the brain. They control which substances can enter the brain and which cannot. This protects the brain from harmful substances and pathogens. The blood-brain barrier is particularly permeable in the case of infectious diseases, certain brain tumors and oxygen deficiency.
Significance for Alzheimer’s, multiple sclerosis and more
“In addition to the blood-brain barrier, the immune cells we studied control what can reach the brain cells from the blood, they eat pathogens and prevent excessive inflammation. They are also involved in the development of cancer, Alzheimer's disease and multiple sclerosis. Our findings could be important for a better understanding of these diseases and future therapies,” Prinz adds.
Color-coded cells and gene analyses Farbmarkierte Zellen und Gen-Analysen
For their study, the researchers led by the two first authors Dr. Takahiro Masuda from Kyushu University, Japan, and Dr. Lukas Amann from the Faculty of Medicine at the University of Freiburg used several newly established mouse lines. With these, different types of brain macrophages and their progenitor cells could be specifically labeled for the first time and later found in the different brain regions using high-resolution microscopy. In addition, they examined the gene activity of individual cells and thus determined their degree of maturity. “We were also able to confirm the data on human brains. This gives us a much deeper understanding of the timing and molecular mechanisms in the development of the cells. This knowledge can now be used to explore new and more specific therapeutic approaches for brain diseases,” says biologist Dr. Lukas Amann, who works at the Institute of Neuropathology at the Medica Center – University of Freiburg.
Researchers from Freiburg, Berlin, Hannover, Leipzig, Japan, Sweden, France and the USA were involved in the study.
Original publication
Masuda, T., Amann, L., Prinz, M. et al. (2022): Specification of CNS macrophage subsets occurs postnatally in defined anatomical niches. In: Nature.DOI: 10.1038/s41586-022-04596-2
Contact:
Prof. Dr. Marco Prinz
Medical Director
Institute of Neuropathology
Medical Center – University of Freiburg
Tel: 0761 270-51060
e-mail: marco.prinz(at)uniklinik-freiburg.de
Bastian Strauch
Office of University and Science Communications
University of Freiburg
Tel.: 0761/203-4301
e-mail: bastian.strauch(at)zv.uni-freiburg.de



